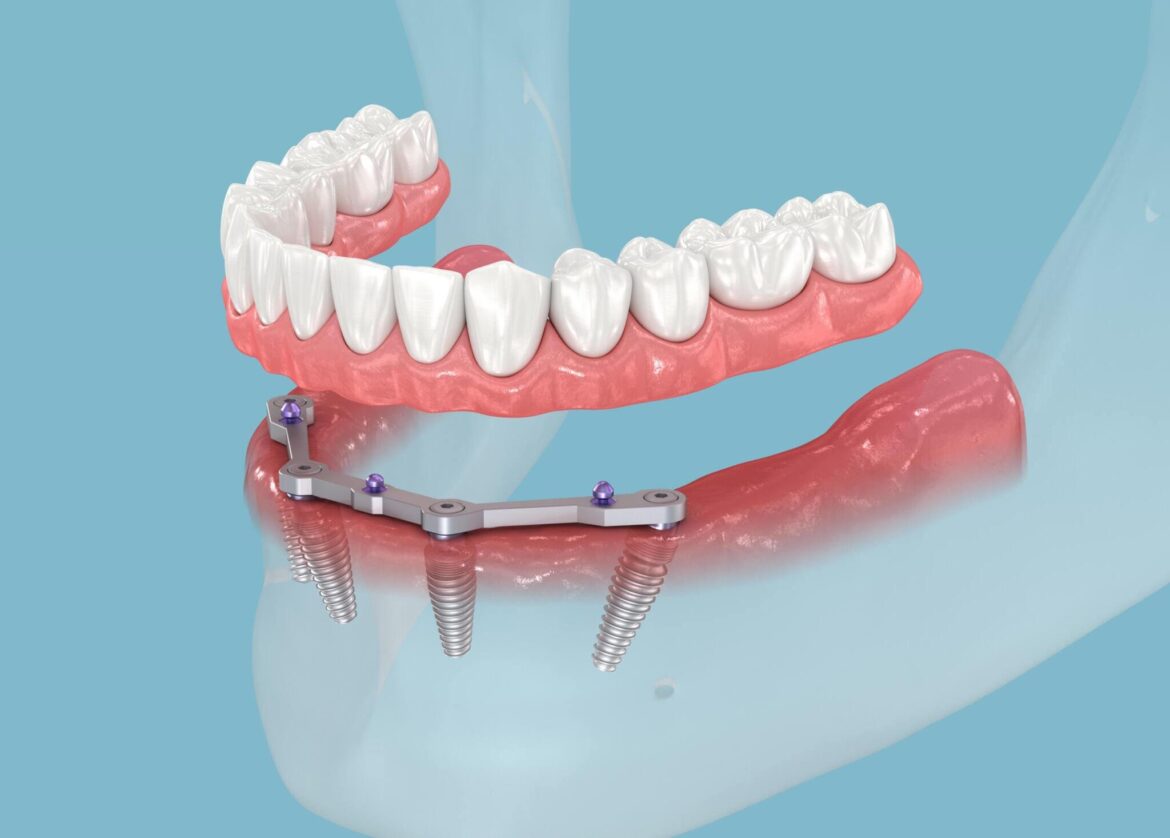
The Marvel of Modern Dentistry
The human jaw possesses a remarkable ability that has revolutionised modern dentistry: the capacity to welcome foreign materials and transform them into permanent fixtures. This extraordinary biological process, known as osseointegration, represents one of the most significant breakthroughs in oral healthcare, particularly in the field of dental implants Northern Ireland and beyond. The science behind bone integration has opened doors to treatments that were once considered impossible, offering patients a second chance at complete oral functionality.
Understanding how titanium posts become living parts of the jawbone requires delving into the intricate world of cellular biology and biocompatibility. When a dental implant is placed, it initiates a complex cascade of healing responses that ultimately determine the success of the procedure. This process challenges traditional notions of how the body accepts foreign materials, demonstrating that with the right conditions and materials, integration rather than rejection becomes the norm.
The Biological Foundation of Osseointegration
The journey of bone integration begins at the microscopic level, where specialised cells orchestrate a symphony of healing and growth. Osteoblasts, the bone-building cells, play a crucial role in this process by depositing new bone material directly onto the implant surface. Meanwhile, osteoclasts work to remodel existing bone tissue, creating space for new growth and ensuring optimal integration patterns.
The surface properties of dental implants have been meticulously engineered to encourage this biological response. Titanium’s unique biocompatibility stems from its ability to form a stable oxide layer that the body recognises as non-threatening. This oxide layer acts as a bridge between the implant and surrounding bone tissue, facilitating the attachment of proteins and cells essential for successful integration.
Factors Influencing Integration Success
Material Science and Surface Technology
The evolution of implant materials has been driven by extensive research into osseointegration mechanisms and bone healing processes. Modern implants feature sophisticated surface treatments that enhance bone-to-implant contact. These modifications include sandblasting, acid etching, and plasma spraying techniques that create micro-textures promoting cellular adhesion and proliferation.
The geometry and thread design of implants also significantly impact integration outcomes. Engineers have developed precise specifications for thread pitch, depth, and angle to optimise primary stability whilst minimising stress concentration points that could compromise long-term success.
Surgical Precision and Timing
The surgical placement technique fundamentally influences the integration process. Maintaining appropriate temperatures during drilling prevents thermal necrosis of bone cells, whilst achieving optimal torque values ensures adequate primary stability without over-compression of surrounding tissues. The healing period following placement allows for the gradual transformation from mechanical retention to biological integration, typically requiring several months for completion.
The Timeline of Bone Integration
The osseointegration process unfolds in distinct phases, each characterised by specific cellular activities and structural changes. During the initial inflammatory phase, lasting approximately one week, blood clot formation and initial healing responses establish the foundation for subsequent bone growth. This phase transitions into the proliferative stage, where new blood vessels form and primitive bone matrix begins to develop around the implant surface.
The maturation phase represents the most critical period, typically extending from six weeks to several months post-placement. During this time, woven bone gradually transforms into mature lamellar bone, creating the strong mechanical connection essential for long-term implant stability. Understanding implant integration mechanics reveals how this biological process creates bonds stronger than those found in natural tooth attachment.
Advances in Integration Technology
Surface Modifications and Coatings
Contemporary research has introduced innovative surface treatments that accelerate and enhance bone integration. Hydroxyapatite coatings mimic natural bone mineral composition, whilst bioactive glass surfaces release ions that stimulate osteoblast activity. These developments have significantly reduced healing times and improved success rates, particularly in challenging clinical scenarios involving compromised bone quality.
Nanotechnology applications have further refined implant surfaces at the molecular level. Nanostructured surfaces increase the available area for cellular attachment whilst providing topographical cues that guide bone cell behaviour and orientation during the healing process.
Growth Factor Integration
The incorporation of biological growth factors represents a frontier in implant technology. Bone morphogenetic proteins and platelet-derived growth factors can be applied to implant surfaces or incorporated into surrounding grafting materials, enhancing the natural healing response and promoting more robust integration outcomes.
Future Perspectives in Bone Integration
The science of osseointegration continues to evolve, with researchers exploring smart materials that respond to biological signals and adapt their properties throughout the healing process. Advanced osseointegration research suggests that future implants may incorporate antimicrobial properties and drug delivery systems to further optimise integration success.
The remarkable science behind bone integration has transformed dental implants into highly predictable treatments. As understanding of cellular mechanisms deepens and technology advances, the barriers between artificial and natural continue to dissolve, offering patients increasingly sophisticated solutions for tooth replacement that truly become part of their biological framework.